Banking & Insurance
< Back to the cases
With 200,000 policyholders, 460,000 health beneficiaries, and 23 partner companies, Verspieren, a major player in insurance brokerage in France, handles a high volume of requests every day.
Behind these figures are often urgent or sensitive calls, a strong reliance on the phone as the primary channel, and customer journeys that can be complex to manage. Teams are heavily engaged, which can lead to longer response times and a less seamless experience for policyholders.
In this context, Verspieren needs to rethink its contact journeys. The challenge is twofold: enabling policyholders to get quick and simple answers, while better controlling flows and team workload.
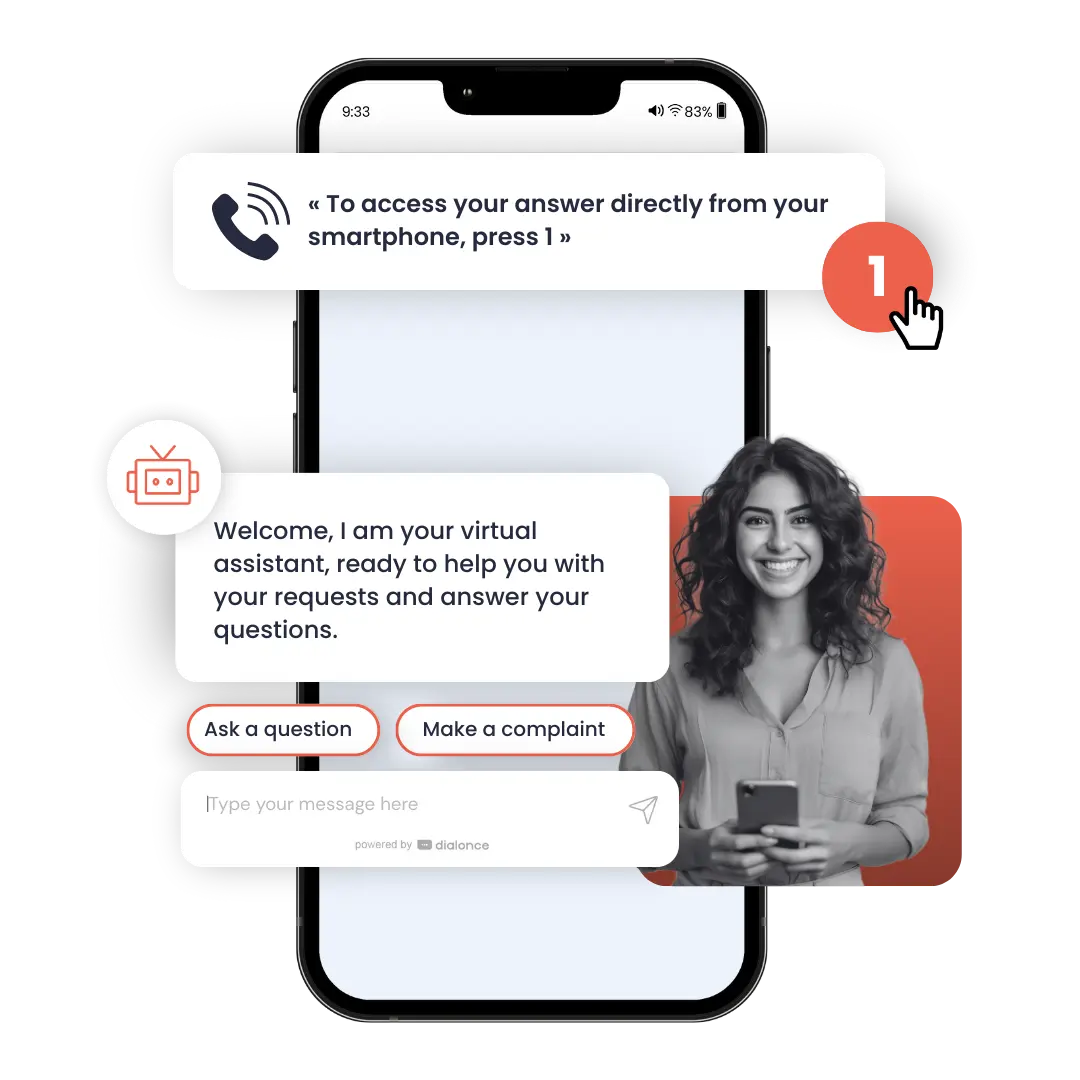
Policyholders today expect immediate, simple, and accessible answers, regardless of their entry point. In insurance, these expectations are even stronger, as requests often relate to important personal situations.
Each interaction therefore needs to be contextualized, simplified, and guided toward the most relevant solution. Without clearly structured journeys, users quickly face long wait times, multiple transfers, or difficulty finding the right information.
The challenge for Verspieren is to make each journey simpler, faster, and more efficient, while still preserving access to a human advisor when needed.
"Provide fast, high-quality responses to our policyholders’ requests. For us, as for most of our corporate clients, the priority is to deliver a successful customer experience. And that starts with providing quick, high-quality responses to policyholders’ needs."
Mylène Béard
Digital and Operational Marketing Manager at Verspieren
After nearly two years of use, Visual IVR is now fully embedded in Verspieren’s strategy. It strikes the right balance between innovation, operational performance, and service quality, while meeting policyholders’ expectations for speed and simplicity.
The solution sustainably structures contact journeys, promotes digital services, and simplifies access to information. It also helps better direct requests, streamline call handling, and increase policyholder autonomy. At the same time, it enables teams to focus on more complex, higher value-added requests.